Reconstructive Procedures
Jump To
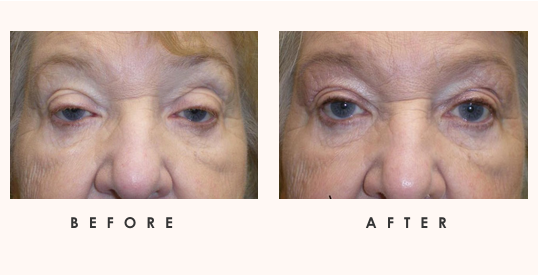
Reconstructive procedures for the face and eyes are often life-changing for patients experiencing functional issues as well as those with cosmetic concerns. At Idaho Eyelid & Facial Plastic Surgery in Boise, reconstructive procedures for the eyes and face are performed by our extensively trained and experienced oculofacial plastic and reconstructive surgeons.
With their expertise in reconstructive oculofacial surgery and their dedication to patient safety, our surgeons have transformed countless patients’ lives, helping them see better and enjoy an improved quality of life.
What Conditions Can Reconstructive Procedures Treat?
At Idaho Eyelid & Facial Plastic Surgery, our surgeons offer reconstructive procedures to address a wide range of conditions, including:
What to Expect Before and After Your Reconstructive Procedure
Prior to your procedure, you will be given important preparation instructions. These will vary depending on your treatment plan but often include abstaining from blood thinners, ibuprofen, and alcoholic beverages for a few days or more before your procedure, as well as ceasing smoking for an extended period of time.
Reconstructive procedure recovery timetables and aftercare requirements differ in relation to the treatment(s) performed. However, in every case, carefully following all aftercare instructions provided is absolutely vital to promote expedient healing and an optimal treatment outcome.
How Much Do Reconstructive Procedures Cost?
The total cost of your reconstructive procedure will depend on the specifics of your treatment plan. The price of your treatment will be impacted by the procedure(s) performed, the complexity of your procedure, anesthesia fees, and other factors.
Learn More about Reconstructive Oculofacial Procedures
If you are ready to reclaim functionality and/or resolve aesthetic concerns associated with an eye or facial condition, reach out to Idaho Eyelid & Facial Plastic Surgery to schedule a consultation. Our practice is proud to offer reconstructive procedures to Boise patients, as well as patients throughout the greater Treasure Valley area.