Pseudotumor
Jump To
Definition
Meaning “false tumor”, the pseudotumor is an idiopathic orbital inflammatory disease caused by increased pressure around the brain. It is a hypo cellular lymphoid lesion, often incompletely replacing the orbital fat, lacrimal gland and extraocular muscles in which mature lymphocytes, plasma cells, histiocytes are seen. The symptoms of pseudotumor cerebri can negatively impact vision.
Demographics
Males and females are equally affected. Both children and adults could be afflicted by idiopathic inflammations. It is most common in middle-aged adults, but also in young children and elderly patient. In children, approximately one-third of cases are bilateral. Bilateral pseudotumor in adults is less common and should elicit evaluation for systemic vasculitis such as Wegener’s granulomatosis or polyatertitisis nodosa) and lymphoma.
Etiology
The etiology of idiopathic orbital inflammation is unknown. It is believed to be an orbital immune reaction, although no local autoantigens in the orbit have been identified. Possibilities include a blood-borne antigen or antibody localizing in the orbit, which has a rich vasculature.
Signs and Symptoms
The clinical presentation is dominated by inflammatory signs and could be variable. The acute form of the disease is the most striking. Pseudotumor cerebri signs and symptoms might include severe headaches that might originate behind the eyes, whooshing sound that pulses with the heartbeat, nausea, vomiting or dizziness, vision loss, and/or brief episodes of blindness, lasting a few seconds and affecting one or both eyes. More clinical signs and symptoms are listed below.

Signs
- proptosis (probably the most frequent cause of following thyroid)
- restricted eye-movement
- conjunctival vascular congestion and edema
- eyelid erythema and swelling
- impaired vision
- decreased corneal sensitivity (CNV1)
- elevated IOP
- intraocular: retinal and choroidal striae, optic nerve hyperemia and swelling, uveitis, and exudative retinal detachment
Symptoms
- constitutional symptoms (especially in children)
- painful ophthalmoplegia
- acute or recurrent, orbital pain
- double vision
Work-up
It is important to evaluate a patient’s history or prior episodes. Orbital CT scans may be needed to determine whether the posterior sclera has thickened. Orbital fat or lacrimal-gland involvement should be assessed along with thickening of the extraocular muscles. In cases of orbital pseudotumor, bone destruction is uncommon.
Differential diagnosis
The differential diagnosis of orbital pseudotumor includes orbital cellulitis, ruptured dermoid cyst, vasculitis (Wegeners’), lymphangioma, lymphoid tumor, and, in children, rhabdomyosarcoma, metastatic neuroblastoma, and Ewing’s sarcoma. In the myocitic subtype, one must also consider thyroid orbitopathy; of note, in thyroid disease, the onset is usually slower, and although asymmetrical, it is often bilateral. Also in the differential in patients with enlarged extraocular muscles are metastatic carcinoma, direct carotid cavernous fistula, spontaneous dural cavernous fistula, and systemic lupus erythematous.
Classification of Psuedotumors
Rootman and Nugent classified acute orbital pseudotumors according to their orbital location, and described five patterns: anterior, diffuse, apical, myositic, and lacrimal.
Anterior
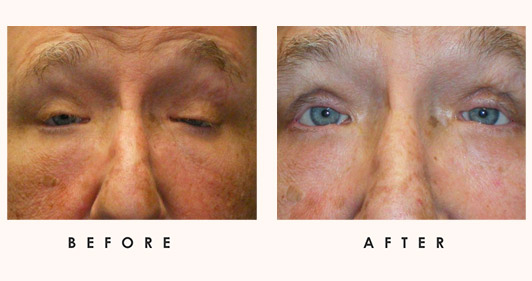
An anterior pseudotumor is inflammation involving the globe and anterior orbit with pain, lid swelling, ptosis. Ptosis is may also be called blepharoptosis, and refers to an eyelid which is droopy. This could cause a loss of vision, especially while reading, headaches, and eyebrow strain (please see the Ptosis page for more details). Also present may be diplopia, uveitis, papillitis, optic neuropathy, and exudative retinal detachment. CT reveals diffuse anterior orbital inflammation, scleral and choroidal thickening.
Diffuse
A diffuse pseudotumor is inflammation similar to anterior pseudotumor but is more severe. Patients could exhibit more severe papillitis, choroiditis, and optic neuropathy. CT reveals diffuse orbital involvement.
Apical
Patients with posterior pseudotumors present with less proptosis, pain, and visible inflammation, but with a tendency toward the early development of optic neuropathy. CT reveals inflammatory process in the orbital apex, possibly extending along the course of the extraocular muscles.
Myositic
Patients with myositic pseudotumors have one or more inflamed extraocular muscles. They often complain of sudden onset of retrobulbar pain, worsened with movement. CT scan reveals diffuse enlargement of the extraocular muscle, including the insertion; in contrast, patients with thyroid ophthalmopathy have enlarged muscles, but sparing the insertion.
Lacrimal
Patients with posterior lacrimal pseudotumors present with less proptosis, pain, and visible inflammation, but with a tendency toward the early development of optic neuropathy. CT reveals inflammatory process in the orbital apex, possibly extending along the course of the extraocular muscles.
Pathology
- The histopathologic findings in pseudotumor are variable, depending on where the biopsy was taken and when in the course of the disease it was sampled.
- Classically, it is composed of 1) an infiltrate including lymphocytes plasma cells, macrophages, eosinophils, and rarely neutrophils 2) follicular lymphoid hyperplasia within a loose fibrous stroma.
- Tissue that is more fibrous is seen in chronic situations. Children could exhibit a heavy eosinophilic infiltrate.
Treatment
- In several cases, treatment of orbital pseudotumor could be initiated without a preceding orbital biopsy. Initial therapy consists of systemic corticosteroids adjusted for the patient’s weight; typically 60- 100 mg/day of prednisone per day. In general, acute cases respond more rapidly than chronic cases and bilateral cases could require a longer course than unilateral disease.
- Additionally, topical Predforte (1% Q.I.D. ) eye drops could be used to treat anterior chamber reaction.
- A biopsy (with touch prep) is performed, however, if there is no clinical improvement after treatment with systemic steroids. Once the diagnosis is confirmed, additionally modalities of therapy include orbital irradiation (low-dose supervoltage radiation in the range of 1000 to 2000 rad is given in divided doses over a 10- to 15-day course) (101)., cyclophosphamide, and rarely orbital decompression.