Horners Syndrome
Jump To
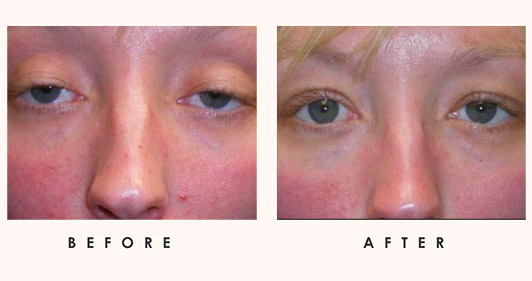
Horner’s syndrome is a rare unilateral condition impacting the nerves that control the eyes, eyelids, and sweat glands. This condition involves a disrupted nerve pathway on one side from the brain to the face and eye. It can arise from strokes, tumors, or spinal cord injuries and is caused by damage to the sympathetic nervous system. Symptoms can include droopy upper lids, some elevation of lower lids, constricted pupils, and delayed dilation. It can also result in the impression that the eye is sunken. Moreover, dilated blood vessels can cause flushing on the impacted side of the face. Horner’s syndrome may lead to different eye colors in children. Prevention strategies include avoiding trauma, controlling cardiovascular risk factors, and stopping smoking.
At Idaho Eyelid and Facial Plastic Surgery, our practitioners work with patients on treatment plans to address the underlying causes of Horner’s Syndrome. The goal is to restore normal nerve function. If a tumor or another condition is the cause, treatment for that condition may resolve the symptoms. However, in some cases, the symptoms may be permanent.
Pathophysiology
Horner’s syndrome typically results from a problem with the sympathetic nerves that lead to the eyes. These nerves are either blocked or damaged by a number of conditions, such as: ear infections, tumors, central lesions involving the spinal cord, or ganglionic lesions. While preganglionic lesions involve sympathetic chain compression (caused by a lung tumor), postganglionic lesions involve the carotid arteries.