Neurofibroma
Jump To
Description of Orbital Neurofibroma
Neurofibromas are rare and represent roughly 3% of orbital tumors. A neurofibroma is recognized as a peripheral nerve sheath neoplasm created by Schwann cells, perineural cells, and fibroblasts. Three subclassifications include: plexiform, diffuse, and localized neurofibromas. Plexiform neurofibroma is more related to neurofibromatosis than diffuse or localized neurofibroma.
Symptoms and Signs of Orbital Neurofibroma
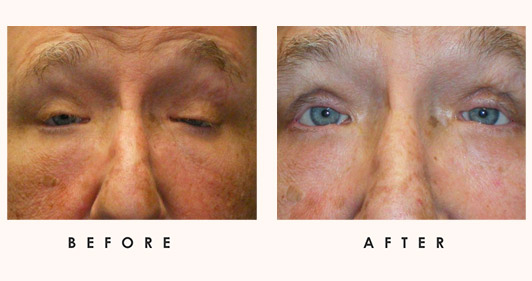
Neurofibromas are suspected when patients present with painful, well-developed orbital tumors. Typical symptoms include an orbital mass, proptosis, globe displacement, impaired extraocular movement, ptosis, and numbness. More specifically:
- Plexiform orbital neurofibroma presents mostly in patients in their first ten years of life, sometimes along with clear indications of neurofibromatosis. Roughly 2/3 of these children have associated eyelid issues.
- Diffuse orbital neurofibroma presents similarly to plexiform neurofibroma. It typically involves unilateral proptosis and involves the eyelids. It is less linked to neurofibromatosis (than plexiform neurofibroma).
- Localized orbital neurofibroma presents in young or middle-aged patients as solitary, well-developed soft tissue tumors. This may coincide with proptosis and downward globe displacement, and can also involve the lacrimal gland, the extraocular muscle, or cause bony destruction.
 Diagnosis of Orbital Neurofibroma
Diagnosis of Orbital Neurofibroma
At Idaho Eyelid and Facial Plastic Surgery, CTs and MRIs may be ordered to confirm diagnosis of orbital neurofibromas. These images may show smoothly marginated ovoid lesions.
Treatment of Orbital Neurofibroma
Orbital neurofibroma treatment at Idaho Eyelid and Facial Plastic Surgery revolves around surgical excision. Removal of localized orbital neurofibroma is possible in roughly 46% of cases (isolated orbital neurofibroma) and has a low recurrence rate, however, 72% of patients reported a sensory skin deficit after surgery. Both plexiform and diffuse orbital neurofibromas are more complicated. For patients with eyelid ptosis and permanent vision loss, orbital reconstruction with an attempt to save the eyelid is the conventional approach. Diffuse infiltration and intracranial involvement make surgery complex. Recurrence after incomplete surgical removal can occur, and follow-up visits are critical.


 Diagnosis of Orbital Neurofibroma
Diagnosis of Orbital Neurofibroma