Blepharospasm
Jump To
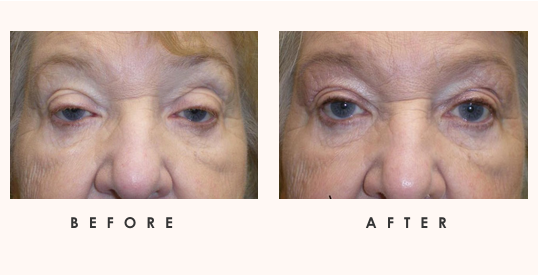
Blepharospasm
Blepharospasm is an involuntary, sustained twitching of the eyelids. It is a condition caused by uncontrolled muscle contraction and is often associated with headaches, eyebrow strain and occasionally loss of vision. Blepharospasm can also coincide with lower facial spasms as part of a syndrome or disease complex, such as:
- Meige Syndrome – characterized by spasm of the eyelids and midface (see video).
- Brueghel’s Syndrome – presents with blepharospasm and marked spasms in the lower face and neck.
- Segmental Cranial Dystonia – in addition to eyelid and facial muscle spasms, this condition is associated with spasms along cranial nerves, most often involving the facial nerve.
- Generalized Dystonia – presents with spasms across various body parts in addition to blepharospasm and facial spasms.
History
For over five centuries, those suffering with blepharospasm and lower facial spasm were institutionalized in mental asylums. This unfortunate practice continued until a breakthrough was made by Henry Meige, a French neurologist in the early 20th century. Meige significantly contributed to the medical field with new findings related to blepharospasm diagnosis and treatment.
Types of Blepharospasm
Blepharospasm occurs in two forms: 1) essential/spontaneous blepharospasm is a rare focal dystonia without any known cause; 2) reflex blepharospasm is due to reflex sensory stimulation through branches of the trigeminal nerve. More information is provided below:
- Essential/spontaneous blepharospasm impacts patients between 45 and 65 years of age and is commonly associated with stress and fatigue. The symptoms can be benign and transient, or can cause significant lifelong challenges. In rare cases, it can result in functional blindness.
- Reflex blepharospasm may be associated with conditions like phlyctenular conjunctivitis, interstitial keratitis, corneal foreign body, corneal ulcers and iridocyclitis. It causes pain in and around the eye may be brought on by excessive stimulation of the retina by dazzling light.
Pathophysiology of Blepharospasm
Blepharospasm is a neuropathologic disorder, the cause of which is multifaceted and not associated with a single central regulatory area in the basal ganglia, midbrain or brainstem. Currently, blepharospasm is thought to be linked with defective blinking circuitry, when corneal or eyelid irritation, pain, emotion, stress and other nerve stimulants trigger the sensory limb of the circuit. Sensory stimuli are transmitted to a defective control center in the midbrain which may be weakened by age, injury or genetics. This defective center results in a failure to regulate the positive feedback mechanism. Abnormal positive feedback signals go unregulated in the motor pathway. This lack of regulation causes uncontrolled muscular contractions in the distribution of facial nerve and its nucleus.
Clinical Presentation of Blepharospasm
Blepharospasm presents as a gradual increase of blinking in response to innocuous stimuli in the environment. This can include wind, polluted air, sunlight, and/or noise. It initially starts in one eye but progresses gradually to involve both eyes and even the facial and neck muscles. Symptoms may include: dry eyes, increased rate of blinking, spasms of the eyelids, irritation of the eyes, eye pain, midfacial or lower facial spasms, brow spasms, and/or eyelid tics. Blepharospasm can present with long-term anatomic changes, such as ptosis, dermatochalasis, entropion, and/or canthal tendon abnormalities.
Blepharospasm is often misdiagnosed. It is sometimes confused with Bell’s Palsy, Allergic conjunctivitis, Dacryocystitis, eyelid myokymia, Keratoconjunctivitis sicca, and Non-granulomatous anterior uveitis. These conditions should be considered in the differential diagnosis while evaluating a suspected case of blepharospasm.
Ideal Candidates
Blepharospasm treatment involves injecting neuromodulators (or botulinum toxin) to reduce or eliminate involuntary eyelid spasms. While this is not a definitive cure, such treatment can effectively manage symptoms. Ideal candidates for neuromodulators injections (like Botox, Dysport, and Xeomin) typically include patients experiencing discomfort, pain, or impaired vision due to blepharospasm. If you have been diagnosed with this condition and are seeking a non-invasive solution to alleviate your symptoms, you may be an excellent candidate for neuromodulator treatment at Idaho Eyelid and Facial Plastic Surgery.
Consultation
A thorough consultation is the first step toward receiving neuromodulator injections for blepharospasm treatment. During this appointment, Idaho Eyelid and Facial Plastic Surgery will assess your medical history, discuss your symptoms, and conduct a comprehensive examination of your eyelid muscles. This evaluation will help determine the severity of your condition and the appropriate injection sites and dosages.
Aftercare
After receiving neuromodulator injections to control eyelid twitching associated with blepharospasm, you may experience mild swelling, bruising, or redness at the injection sites, but these side effects typically resolve within a few days. It’s essential to follow the post-treatment care instructions to ensure proper recovery.
Cost
The cost of neuromodulator injections for blepharospasm varies depending on factors such as the severity of your condition and the number of injections needed. It’s important to note that in some cases, health insurance may cover the cost of these treatments, so be sure to check with your insurance provider.
Contact Us
If you’re seeking relief from blepharospasm in the Treasure Valley through neuromodulator injections, our experienced medical team is here to best assist you. To schedule a consultation or inquire about the treatment, contact Idaho Eyelid and Facial Plastic Surgery. We are committed to helping you regain comfort, confidence, and control over your life by providing effective solutions for blepharospasm.