Lacrimal System
Jump To
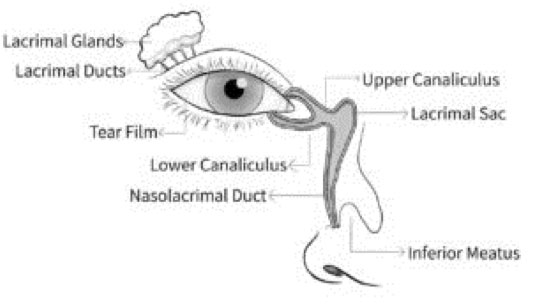
The lacrimal system is crucial for maintaining eye health. It includes structures responsible for tear production and drainage. Tears lubricate the eye’s surface, remove debris, and protect against infection. Prioritizing its care is essential for optimal eye health.
Anatomy of the Lacrimal System
The lacrimal system includes the lacrimal glands and tear ducts. These glands, located above each eyeball, release lacrimal fluid onto the eye’s surface. This fluid nourishes and lubricates the eyes, forming tears when produced in excess. The gland has two parts: orbital and palpebral. Within the gland, lobules contain serous cells that produce watery secretions. Tear drainage occurs through a network of ducts that lead into the nasal cavity.
Importance of the Lacrimal System
The lacrimal system plays a vital function in distributing tears evenly across the eye and ensuring proper drainage. It begins with the lacrimal punctum, continues through canaliculi in the eyelids, and ultimately drains into the lacrimal sac. From there, tears travel through the intra-osseous lacrimal duct and exit into the nasal cavity. Obstruction in this system can cause excessive tearing.
Common Lacrimal System Disorders
Disorders affecting the lacrimal system can significantly impact eye comfort and functionality. Among the most prevalent issues are:
- Blocked Tear Ducts: This condition prevents tears from draining normally, leading to watery eyes and increased risk of infection.
- Tear Duct Obstruction: Similar to blocked tear ducts, this involves a blockage that impedes tear flow, causing discomfort and excessive tearing.
- Dacryocystitis: An infection of the lacrimal sac, primarily due to obstruction in the tear duct, resulting in pain, redness, and swelling near the eye.
- Dry Eye Syndrome: Although not a direct disorder of the tear ducts, it’s related to inadequate tear production or poor tear quality, leading to eye irritation and blurred vision.
- Canaliculitis: An infection of the canaliculus (a part of the tear drainage system), causing redness, pain, and discharge from the eye.
- Dacryostenosis: A narrowing of the tear duct that can lead to blockages, affecting tear drainage and causing symptoms similar to those of blocked tear ducts.
- Lacrimal Gland Tumors: Though rare, tumors of the lacrimal gland can affect tear production and drainage, leading to a range of symptoms, from discomfort to vision impairment.
These conditions can disrupt daily life by causing persistent discomfort and affecting vision clarity. Early diagnosis and treatment are crucial for managing symptoms and preventing complications.
Symptoms and Signs of Lacrimal System Issues
Issues with the lacrimal system manifest through a variety of symptoms, which are crucial for early detection and effective management. Key indicators include:
- Excessive Tearing: An overflow of tears onto the face, often without a clear emotional or irritative cause.
- Watery Eyes: Persistent moisture in the eyes that does not stem from normal tear production.
- Discomfort in the Eyes: Feelings of irritation, scratchiness, or the sensation of a foreign body in the eye.
- Recurrent Infections: Frequent eye infections or inflammation can indicate an underlying issue with tear drainage.
- Blurred Vision: Excessive tears or other related issues can lead to temporary blurring of vision.
- Swelling Near the Eyes: Inflammation or swelling in the areas surrounding the eyes, particularly near the tear ducts.
- Discharge: Unusual discharge from the eyes, which may be clear or contain mucus or pus.
Recognizing these symptoms promptly can facilitate timely consultation at Idaho Eyelid and Facial Plastic Surgery, leading to more effective treatment strategies.
Diagnosis and Testing for Lacrimal System Conditions
The process of diagnosing conditions of the lacrimal system is comprehensive, involving several steps to accurately identify the root cause of symptoms:
- Clinical Examination: A detailed examination of the eye, focusing on the lacrimal system to assess any visible signs of disorder.
- Patient History: Discussion of symptoms, their duration, and any previous eye conditions or surgeries that might influence the current situation.
- Imaging Studies: Techniques such as dacryocystography (DCG) or magnetic resonance imaging (MRI) may be employed to visualize the lacrimal system’s structure and identify blockages or abnormalities.
- Tear Production Tests: Tests measure tear production to evaluate whether tear-related symptoms are due to overproduction or inadequate drainage.
- Probing and Irrigation: A procedure where a thin instrument is used to probe the tear ducts, sometimes combined with the flushing of saline through the system to identify blockages.
These diagnostic measures are useful for developing an effective treatment plan, tailored to address the specific issues of the lacrimal system.
Treatment Options for Lacrimal System Disorders
The approach to treating lacrimal system disorders is tailored to the individual’s condition, ranging from non-invasive methods to surgical interventions:
Conservative Treatments:
- Tear Duct Massage: Gentle massage over the affected tear duct to promote drainage.
- Warm Compresses: Applying warmth to the eye area to alleviate blockages and discomfort.
- Antibiotics: For infections causing or caused by lacrimal system issues, antibiotic drops or ointments may be prescribed.
- Eye Drops: Lubricating eye drops can relieve symptoms of dryness and irritation.
Surgical Treatments:
- Dacryocystorhinostomy (DCR): A procedure to create a new pathway for tear drainage directly into the nasal cavity, bypassing blockages in the tear ducts.
- Tear Duct Probing and Irrigation: For less severe blockages, especially in children, a probe is used to open the duct, often combined with saline irrigation.
- Balloon Catheter Dilation: A minimally invasive procedure where a balloon catheter is used to widen the tear duct and facilitate drainage.
- Intubation of the Tear Ducts: Placement of a small tube to keep the ducts open and ensure proper tear flow.
- Lacrimal Gland Surgery: In cases involving the lacrimal gland, procedures may be necessary to address tumors or severe obstructions.
Lacrimal System Surgery
Lacrimal system surgery, specifically dacryocystorhinostomy (DCR), involves creating a new passage for tears to drain directly into the nasal cavity, bypassing blocked or narrowed ducts.
In the external dacryocystorhinostomy (DCR) approach, a precise incision is made close to the inner corner of the eye. This allows the surgeon access to reroute tear flow around any obstructions. The procedure is aimed at re-establishing efficient tear drainage, which improves symptoms and prevents issues such as excessive tearing and infections.
Recovery and Aftercare
Post-surgical recovery is crucial for the success of lacrimal system procedures. The aftercare regimen may include:
- Follow-up Visits: Regular appointments to monitor healing and ensure the surgery’s success.
- Medications: Use of prescribed antibiotics to prevent infection and anti-inflammatory medications to reduce swelling.
- Eye Care: Instructions on how to care for the eye area, including cleaning and avoiding rubbing or pressure.
- Activity Restrictions: Guidance on activities to avoid during the recovery period to prevent complications.
- Use of Eye Drops: Lubricating drops may be recommended to keep the eye moist and comfortable during the healing process.
Adhering to these aftercare instructions is essential for a smooth recovery and optimal surgical outcome. Patients are encouraged to communicate with our team about any concerns or symptoms that arise during the recovery phase.
When to Consult an Eye Specialist
If you experience symptoms like persistent watery eyes, excessive tearing, discomfort, or recurrent eye infections, consider seeking the expertise of an eye specialist. An early consultation with an ophthalmologist can lead to a timely diagnosis and intervention, improving outcomes and preventing further complications.
Why Choose Us
Idaho Eyelid and Facial Plastic Surgery specializes in resolving lacrimal system issues. Our team of renowned ophthalmologists is dedicated to providing expert care. We utilize state-of-the-art diagnostic tools and offer advanced treatment options tailored to each patient’s specific needs. Our commitment extends beyond effectiveness; we prioritize personalized care, ensuring that every individual receives the necessary support and attention for optimal eye health.
Schedule A Consultation
If you need more information or want to schedule a consultation regarding lacrimal system care in Boise, feel free to reach out to our team at Idaho Eyelid and Facial Plastic Surgery. We are here to address any questions or concerns you may have, ensuring the well-being of your eyes. Schedule a consultation today.