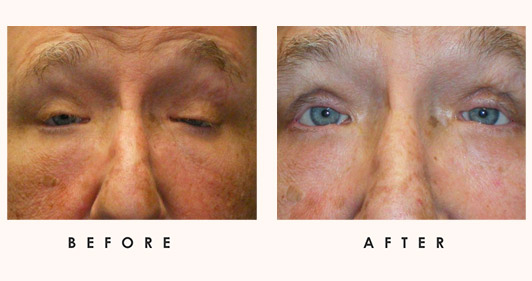
Lacrimal Infections
Jump To
At Idaho Eyelid and Facial Plastic Surgery, patients visit us with complains about swelling, pain, and tenderness of the inner eyelid. This can involve a number of conditions, including dacryoadenitis and canaliculitis. These frequently diagnosed conditions are described below, followed by more specific conditions and treatment paths.
Dacryoadenitis
Inflammation of the tear-producing lacrimal gland is called dacryoadenitis and may be caused by infections, autoimmune diseases, or other inflammatory conditions. It can result in swelling, pain, and redness around the outer part of the upper eyelid. Systemic diseases can cause dacryoadenitis. These include Sjogren’s, sarcoidosis, syphilis, tuberculosis, lymphoma, benign lymphoid hyperplasia, and zoster.
Canaliculitis
Canaliculitis is marked by inflammation of the lacrimal canaliculi, the eyelid channels draining tears into the tear sac. It is caused by bacterial, fungal or viral infections, or as a reaction to a foreign body such as a punctal plug. Symptoms include tearing, discharge, redness, and tenderness. It mostly impacts patients over the age of 50 years.
Pathophysiology of Canaliculitis
A common cause of canaliculitis is the bacteria Actinomyces Israelii; however, there are other causes such as aspergillus, Canada albicans and even herpes simplex/zoster virus. Infections form tiny stones rich in sulphur. The stones form little pockets unaffected by the antimicrobial properties of tears.
History and Examination
Patients complain of one eye being red and inflamed. The inner eye may present with a gooey discharge and the lacrimal punctum may appear swollen, inflamed, and tender. When applying pressure, the discharge is expressed through the punctum.
Diagnosis
Patient history and examination helps confirm diagnosis in most cases. Sulphur stones become apparent when a probe is passed through the lacrimal punctum. Discharge material may be sent to a laboratory to determine the type of infection impacting the canaliculus. This may reveal Actinomyces, aspergillus, or other bacteria.
Treatment
Warm compressions, massage, and antibiotic ointments may help the patient. If sterile solution and broad-spectrum antibiotics are ineffective, a straightforward surgical procedure can help clear the infection. This procedure is called a canaliculotomy and involves a small incision on the conjunctival aspect of the canaliculus. The sulphur stones are removed and antibiotics help clear any residual infection.
Conclusion
Canaliculitis is marked by mostly bacterial infections within the canaliculi. Symptoms include pain, swelling, tenderness of the inner canthus. Sulphur stones complicate matters. Treatments involves antibiotics, drainage, and potentially surgical clearance.
Dacryocystitis
Dacryocystitis involves the inflammation of the tear-producing lacrimal gland. Tearing from a nasolacrimal duct obstruction results in redness, discharge, and/or tenderness. Subsequent infection may cause painful swelling in the inner eyelid. In more severe cases, a surgical procedure called a dacryocystorhinostomy (DCR) may be performed. Surgical obstruction removal is performed by creating a new tear duct. Silicone tubes may be inserted to keep the new tear duct open while healing occurs.
Acute Dacryocystitis
Acute dacryocystitis involves the sudden onset of inflammation/infection caused by a nasolacrimal duct obstruction, blocking drainage from the lacrimal sac to the nose. Secondary infections can be caused by chronic tear stasis. Swelling below the medial canthal tendon is possible. Treatment involves warm compresses, topical and oral antibiotics, and drainage. Potential complications include mucocele, chronic conjunctivitis, and/or orbital cellulitis. Many patients require a DCR after acute dacryocystitis subsides.
Chronic Dacryocystitis
Chronic dacryocystitis is a longer-lasting inflammation/infection marked by the buildup of both tears and bacteria. It also involves nasolacrimal duct obstruction. Probing and irrigating the system can yield good results, but treatment usually requires a DCR.