Eye Inflammation
Jump To
Eye inflammation includes a variety of ocular inflammatory conditions that can cause discomfort and affect vision. Early detection and treatment are important to alleviate discomfort and prevent complications such as vision impairment. At Idaho Eyelid and Facial Plastic Surgery, our team provides comprehensive management, blending medical treatments and lifestyle adjustments to mitigate symptoms and address underlying causes effectively.
Common Causes of Eye Inflammation
The common causes of eye inflammation are diverse, each contributing to conditions in unique ways, and understanding these can significantly enhance prevention and treatment strategies.
Allergies are a prevalent cause, with the eyes reacting to allergens such as pollen, dust, and pet dander, leading to symptoms like itching, redness, and watering. Identifying and avoiding these allergens, along with the use of antihistamine eye drops, can effectively manage allergic reactions.
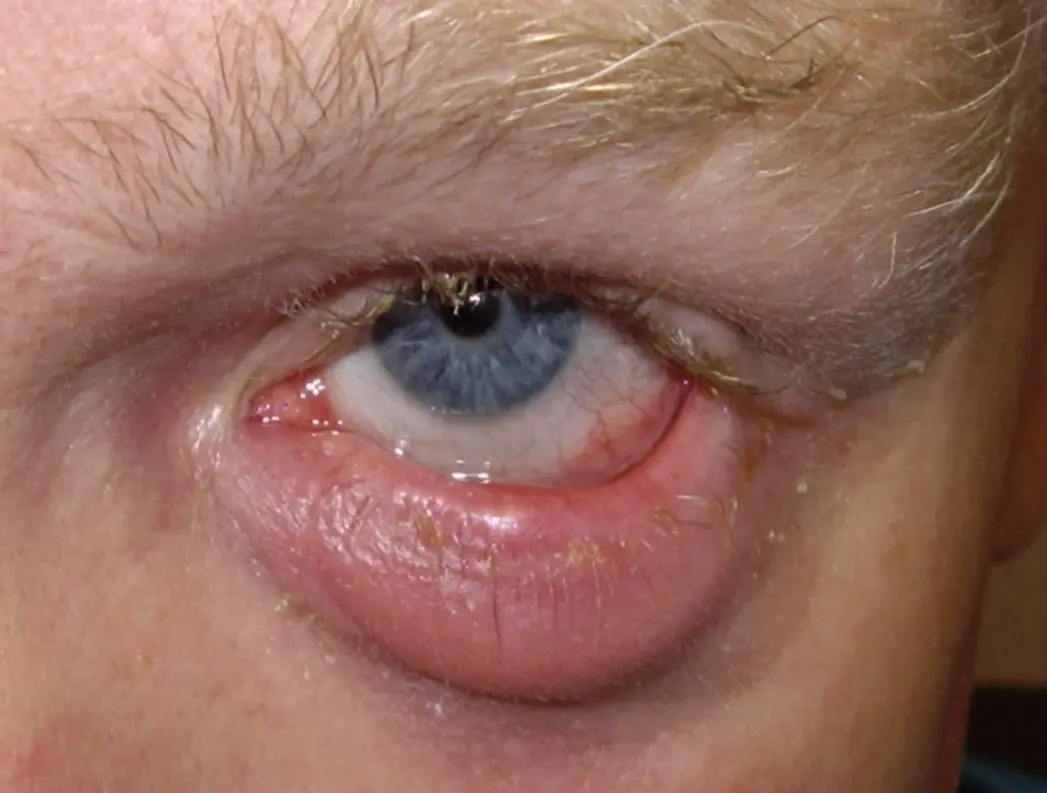 Autoimmune eye diseases, such as rheumatoid arthritis or Sjögren’s syndrome, can lead to inflammation as the body’s immune system mistakenly attacks healthy eye tissues. Managing these conditions often requires systemic medications to control the body’s immune response.
Autoimmune eye diseases, such as rheumatoid arthritis or Sjögren’s syndrome, can lead to inflammation as the body’s immune system mistakenly attacks healthy eye tissues. Managing these conditions often requires systemic medications to control the body’s immune response.
Infections, whether viral, bacterial, or fungal, can cause significant eye inflammation. Viral conjunctivitis and bacterial keratitis are examples where prompt treatment is essential to prevent vision loss. The use of appropriate antimicrobial eye drops or oral medications is critical in these cases.
Exposure to irritants, including chemical vapors, smoke, or even prolonged screen use, can lead to eye inflammation. Protective measures, such as wearing safety goggles or taking regular screen breaks, can help minimize exposure.
Signs and Symptoms of Eye Inflammation
The symptoms and signs of eye inflammation are critical to recognize for timely intervention, which can prevent progression and safeguard vision. Key indicators include:
- Redness. One of the most noticeable signs is when the white part of the eye (sclera) appears bloodshot or pink, indicating irritation or inflammation.
- Swelling. Inflammation can cause the eyelids or surrounding tissues to swell, often accompanied by a feeling of fullness around the eyes.
- Eye Pain. Discomfort ranging from a mild ache to severe pain, often exacerbated by light exposure or blinking, signaling the need for immediate evaluation.
- Impaired Vision. Blurry or decreased vision may occur, as inflammation can affect the cornea or other structures involved in focusing.
- Tearing or Discharge. Excessive tearing or the presence of unusual discharge can be a response to irritation or an attempt by the eye to remove harmful irritants or pathogens.
- Sensitivity to Light. Known as photophobia, this condition where light becomes bothersome or painful is a common consequence of inflammation.
- Itching. Particularly in cases of allergic conjunctivitis, itching can be intense and accompanied by burning sensations.
Early recognition of symptoms allows for timely diagnosis and treatment, preventing complications like corneal damage or vision loss. Treatments, including anti-inflammatory medications, antibiotics, or antihistamines, are tailored to the specific cause of inflammation.
Types of Eye Inflammatory Conditions
There are various inflammatory ocular conditions which can impact the eyelid and the eye. Some of the common ones are listed below.
- Conjunctivitis. Inflammation of the conjunctiva, the membrane covering the white part of the eye and the inner eyelids, often resulting in redness, itching, and discharge.
- Uveitis. Involves inflammation of the uvea, the middle layer of the eye, which can cause pain, blurred vision, and light sensitivity. It requires prompt treatment to prevent vision loss.
- Blepharitis. A condition characterized by inflamed eyelids, leading to red, swollen eyelids, and crusty eyelashes. It’s often associated with an underlying skin condition or bacterial infection.
- Scleritis. A serious condition involving inflammation of the sclera, the white outer layer of the eye, causing severe pain and potentially affecting vision.
- Keratitis. Inflammation of the cornea, the clear front surface of the eye, which can result from infection or injury, leading to pain, redness, and blurred vision.
- Orbital Cellulitis. A severe infection involving the tissues around the eye, leading to pain, swelling, and sometimes vision loss. It requires immediate medical attention.
- Episcleritis. A milder form of scleral inflammation that affects the episclera, causing localized redness and discomfort but usually not affecting vision.
- Endophthalmitis. A severe, potentially vision-threatening infection of the internal parts of the eye, often following surgery or penetrating injury.
Each of these conditions can significantly impact eye health and vision if not properly diagnosed and treated.
Diagnosis and Testing for Eye Inflammation
 Diagnosis and testing for eye inflammation are essential steps to identify the underlying cause and determine the appropriate treatment. These processes involve a combination of ophthalmic exams and specific tests tailored to the symptoms and suspected causes of inflammation.
Diagnosis and testing for eye inflammation are essential steps to identify the underlying cause and determine the appropriate treatment. These processes involve a combination of ophthalmic exams and specific tests tailored to the symptoms and suspected causes of inflammation.
- Clinical Examination. A comprehensive eye exam, including a review of the patient’s medical history and symptoms. The eye doctor may use a slit lamp microscope to examine the structures of the eye in detail.
- Visual Acuity Test. Measures how well the patient can see at various distances, helping to assess the impact of inflammation on vision.
- Tonometry. Measures the pressure inside the eye, which can be affected by certain types of eye inflammation, such as uveitis.
- Slit Lamp Examination. Allows the doctor to examine the front part of the eye under high magnification to identify signs of inflammation, such as redness, swelling, or discharge.
- Dilated Fundus Examination. By dilating the pupils, the doctor can examine the back of the eye, including the retina and optic nerve, for signs of inflammation or damage.
- Blood Tests. May be ordered to identify systemic conditions that could be causing or contributing to the eye inflammation, such as autoimmune diseases.
- Imaging Tests. Techniques like optical coherence tomography (OCT), fluorescein angiography, or ultrasound imaging can provide detailed images of the eye’s structures, helping to pinpoint areas of inflammation or damage.
- Laboratory Analysis of Eye Samples. In cases where infection is suspected, samples from the eye may be taken to identify the specific pathogen causing the inflammation.
These diagnostic tools and tests enable ophthalmologists to accurately diagnose the type of eye inflammation, understand its severity, and tailor a treatment approach that addresses the specific cause and symptoms experienced by the patient.
Treatment Options for Eye Inflammation
Treatment options for eye inflammation are designed to alleviate symptoms, address underlying causes, and prevent potential complications. The choice of treatment depends on the specific type of inflammation and its severity. Here are some common treatments:
- Anit-inflammatory eye drops. These are often the first line of treatment for reducing inflammation and discomfort in the eye. They can be non-steroidal anti-inflammatory drugs (NSAIDs) or corticosteroids, depending on the condition’s severity. NSAID eye drops are used for mild to moderate inflammation, these drops help reduce pain and swelling without the potential side effects of steroids. Corticosteroid eye drops are more potent than NSAIDs, these are used for more severe inflammation. They must be used under close medical supervision due to potential side effects, such as increased intraocular pressure and cataract formation.
- Steroid eye drops. These are crucial for treating different eye inflammations because they strongly reduce inflammation. They work well for uveitis, severe allergic conjunctivitis, and certain types of keratitis. Yet, their usage needs close supervision by an eye specialist due to potential risks like glaucoma, cataracts, and higher chances of infections.
- Oral medication. For more severe cases or systemic conditions affecting the eye, oral medications, including steroids and immunosuppressants, may be prescribed. These can help control inflammation from within and are used for conditions like severe uveitis, scleritis, and systemic autoimmune diseases impacting the eye.
- Immunomodulatory therapy (IMT). In cases where conventional steroids are not effective or suitable, IMT drugs can be used to modulate the immune system’s response, thereby reducing inflammation. These are often used for chronic or severe inflammatory conditions that do not respond well to other treatments.
- Antibiotics/antivirals. If the inflammation is due to an infectious cause, such as bacterial or viral infections, appropriate antibiotics or antiviral medications will be prescribed either in the form of eye drops or systemically.
- Lifestyle. In addition to medical treatments, lifestyle changes such as avoiding known allergens, using warm compresses, and maintaining eyelid hygiene can be beneficial, especially for conditions like blepharitis or meibomian gland dysfunction.
- Surgery. In certain cases, surgical intervention may be necessary to address structural problems contributing to inflammation, such as eyelid abnormalities, or to remove obstructions in the tear drainage system.
The treatment plan should be tailored to the individual’s specific condition and needs, under the guidance of an ophthalmologist.
Managing Chronic Eye Inflammation
Managing chronic eye inflammation requires a comprehensive approach that addresses both the symptoms and the underlying causes to improve quality of life and prevent vision impairment. Effective management strategies focus on long-term treatment plans and preventive measures to control inflammation and minimize flare-ups. For chronic conditions, developing a sustained treatment plan in consultation with an eye care specialist is crucial. This plan may include:
- Regular monitoring. Frequent check-ups allow for adjustments in treatment based on the current state of inflammation.
- Continuous medication. Long-term use of medications, such as immunosuppressive drugs or low-dose corticosteroids, may be necessary to keep inflammation under control.
- Immunomodulatory therapy (IMT): For patients who cannot tolerate steroids or have not responded adequately to them, IMT can offer an alternative to manage inflammation with potentially fewer side effects.
Prevention strategies are key to managing chronic eye inflammation effectively. These include:
- Identifying and avoiding triggers: Understanding what triggers inflammation for the individual patient can help in avoiding those triggers, whether they are environmental allergens, specific activities, or stress.
- Lifestyle modifications: Simple changes, such as wearing sunglasses to protect the eyes from UV light and debris, maintaining good eyelid hygiene, and using humidifiers to keep the air moist, can help reduce the risk of flare-ups.
- Diet and nutrition: A diet rich in omega-3 fatty acids, antioxidants, and other nutrients known to support eye health may also help manage inflammation.
Supportive care measures are also important in managing chronic eye inflammation:
- Artificial tears: For conditions associated with dry eyes, regular use of artificial tear solutions can provide relief from irritation and discomfort.
- Warm Compresses and eyelid massage: These can be particularly beneficial for conditions like blepharitis or meibomian gland dysfunction, helping to relieve symptoms and improve gland function.
Managing chronic eye inflammation is a dynamic process requiring continuous attention and adjustment. Patient education about their condition, treatment adherence, and recognizing flare-up signs are vital. For some, a collaborative approach involving their primary eye care provider and specialists like rheumatologists for autoimmune conditions can offer a more holistic management strategy.
When to Consult an Eye Specialist
It’s important to consult an eye specialist if you experience symptoms of eye inflammation or if preventive measures don’t bring relief. Key indicators for seeking an eye doctor’s evaluation for inflammation include persistent redness, pain, blurred vision, sensitivity to light, or sudden changes in vision. Scheduling an appointment with an ophthalmologist is crucial for a thorough evaluation and an accurate diagnosis.
At Idaho Eyelid and Facial Plastic Surgery, our eye care specialists provide personalized treatment options and management strategies to address the underlying causes of inflammation. Early intervention by a professional can help prevent complications, safeguarding eye health and vision.
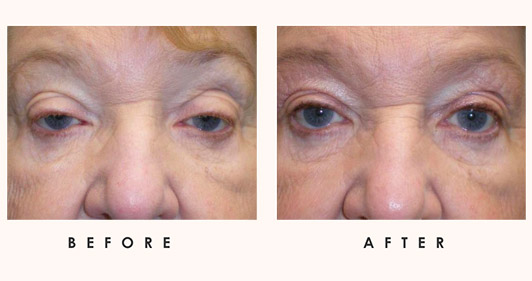
In the context of existing eye inflammation, evaluating the risks and benefits of cosmetic surgery is crucial. Before proceeding with such procedures, it’s important to ensure any active inflammation is fully resolved, as it can complicate surgery and recovery, increasing the risk of infection or poor outcomes.
A comprehensive assessment by an ophthalmologist, in collaboration with a cosmetic surgeon, is essential. This approach prioritizes both cosmetic goals and eye health, minimizing risks and promoting optimal results.
Why Choose Our Clinic for Eye Inflammation
Choosing our clinic for managing eye inflammation means entrusting your eye health to our expert ophthalmologists. We’re dedicated to specialized eye care, delivering personalized treatment plans tailored to each patient’s needs. Our focus on patient education empowers individuals to make informed decisions about their eye health. Our commitment to excellence, combined with our state-of-the-art facilities, makes us a preferred choice for those seeking effective solutions for eye inflammation and other ocular conditions.
Get In Touch
For personalized care and expert management of eye inflammation, we encourage you to contact our eye inflammation specialists at Idaho Eyelid & Facial Plastic Surgery. To request an eye consultation and discuss your specific needs with our team, contact us today.