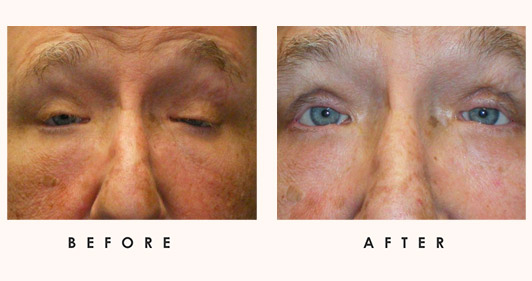
Adult Tumors
Jump To
Introduction to Orbital Tumours
Benign or malignant masses can grow within the bony socket of the eye. They may cause protruding eyeballs (proptosis), vision changes (double vision and blurred vision) along with other symptoms. To detect these tumors, ultrasonography, computerized tomography, and magnetic resonance images are used. The lacrimal gland is responsible for most malignant orbital tumors, which may require biopsy and radical surgery.
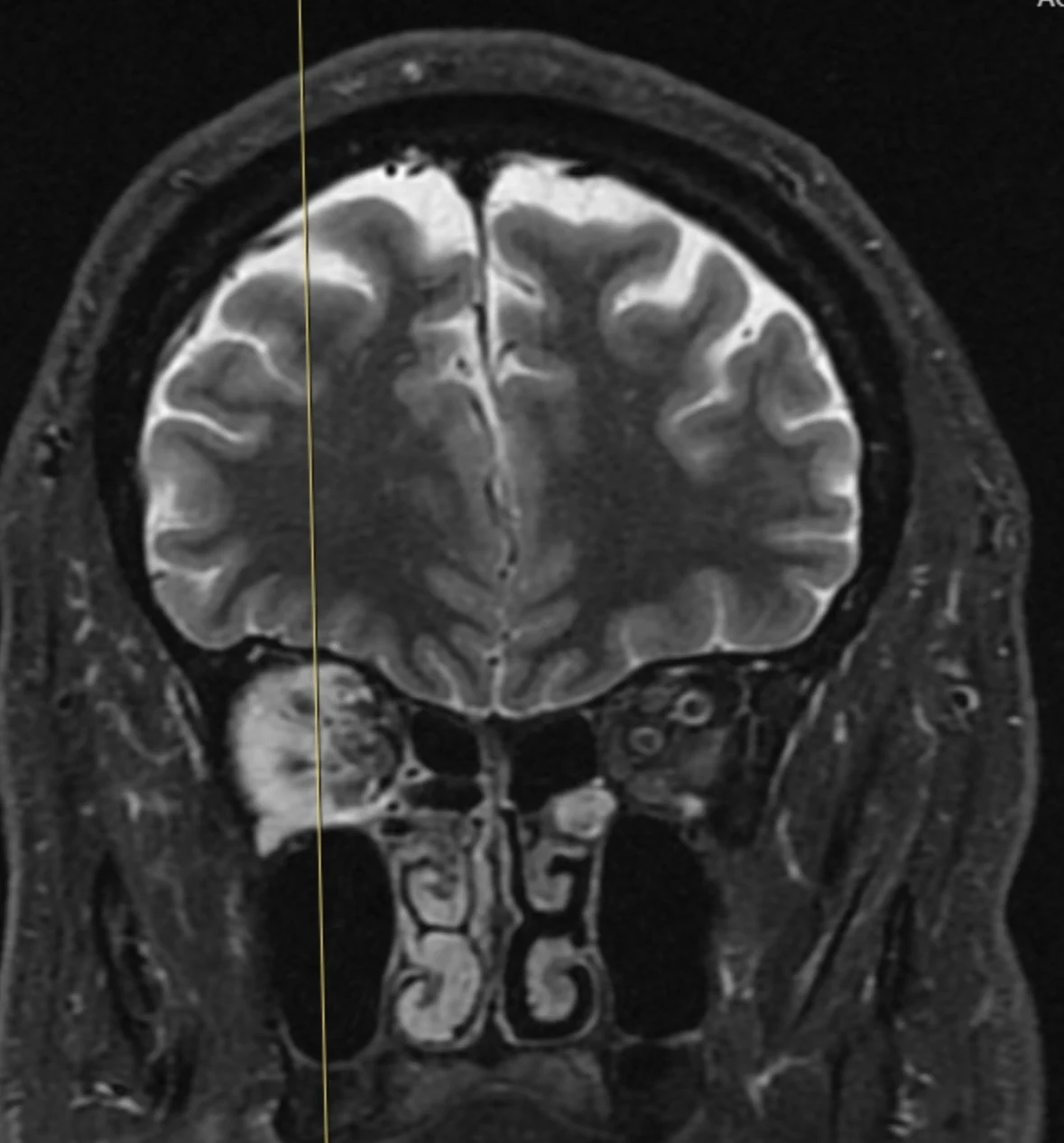
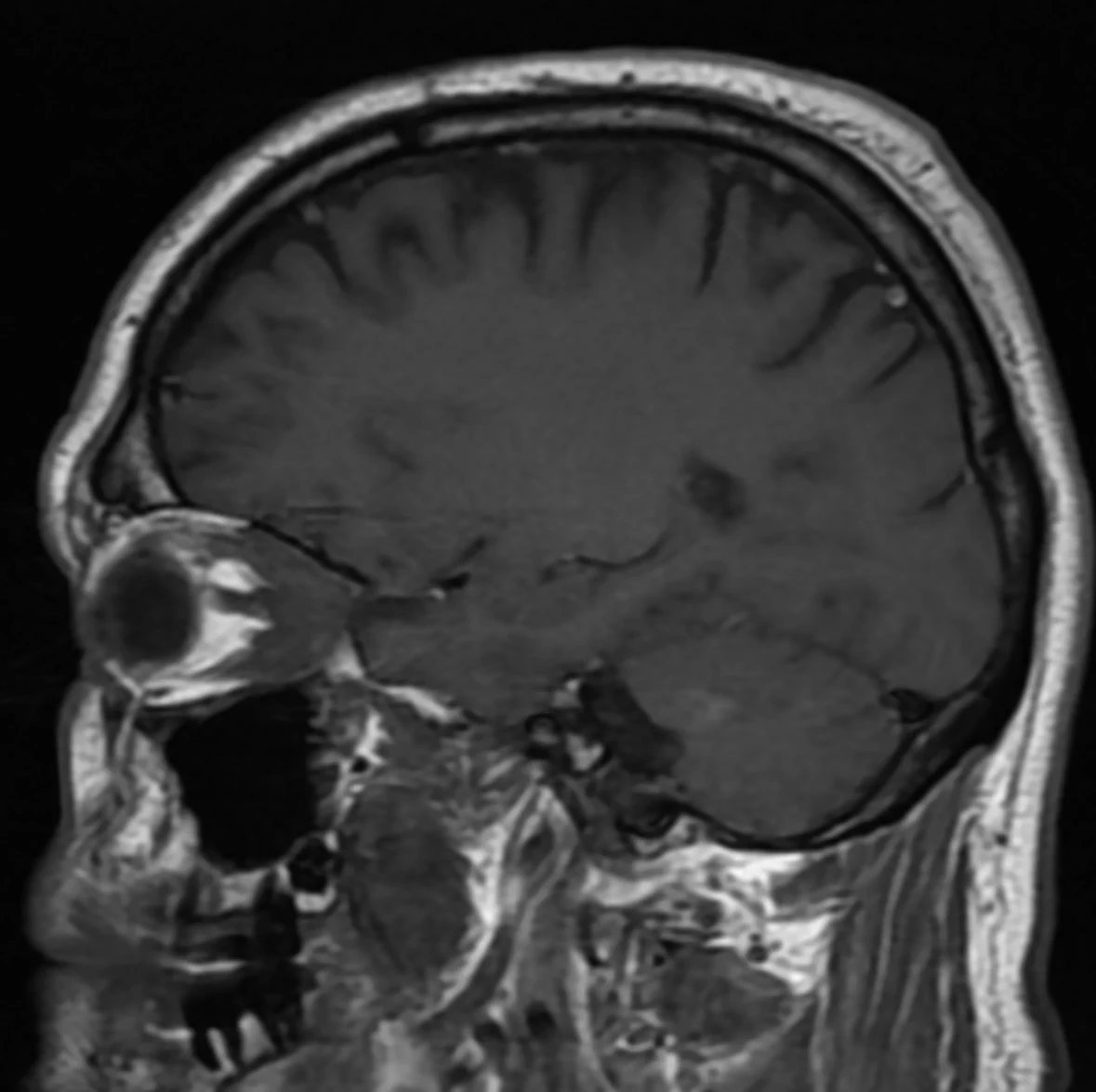
Signs and Symptoms
At Idaho Eyelid and Facial Plastic Surgery, patient symptoms aid us in diagnosing orbital tumors. Protruding or bulging eyeballs due to anterior displacement of the globe is a common sign. This proptosis may cause ptosis, or droopy eyelids. Orbital tumors in the inferior orbit displace the globe vertically, while orbital tumors in the superior orbit displace the globe inferiorly. Growths can impact extraocular muscle movement and nerve function. Patients often experience tenderness and orbital pain. Pain is usually a symptom in patients who have rapidly growing tumors. Patients may also feel pressure on the sensory nerves, resulting in periocular problems. In addition to double vision or blurred vision, a patient’s visual fields may be affected. Eyelid swelling (edema) may result from obstructed venous outflow.
Benign and Malignant Diseases of the Orbit
Orbital tumor growth can be well-defined or diffuse and can involve the thyroid, lacrimal gland, or bones. They can be localized or metastatic from other parts of the body. Well-defined orbital masses, diffuse orbital masses, thyroid-related orbital masses, orbital bony lesions, and lacrimal gland masses are described below.
Orbital masses that are well defined include cavernous hemangioma, neurofibromas, schwannoma, hemangiopericytoma, meningioma, and gliomas. Cavernous hemangioma is one of the most frequently identified benign adult orbital tumors. Patients often experience painless eye bulging/proptosis that progresses over time. Surgical excision is usually the preferred course of action.
Orbital masses that are diffuse may need a biopsy to confirm the diagnosis. Diffuse orbital masses include lymphoma, benign reactive lymphoid hyperplasia, orbital cellulitis, benign or malignant fibrous histiocytoma, neurofibromas, and sarcomas. Of these, lymphangioma, fibrous histiocytoma, and neurofibroma require surgery, while lymphomas often require radiation/chemotherapy treatment.
Thyroid eye disease is an autoimmune condition resulting in inflammation around the eye. It can cause proptosis. Thyroid eye disease is also known as thyroid ophthalmology, and is a common cause of orbital tumors in adults (even with a normally functioning thyroid). It is much more frequent in women, especially those who smoke or are in perimenopause. Anterior eye pain is treated with lubricants and topical steroids. Associated glaucoma is treated through topical anti-glaucoma medications. Proptosis might require steroids, radiation, or corrective surgery.
Orbital bony lesions are diagnosed with CT scans and can be primary or secondary. Primary bony lesions include osteomas, osteogenic sarcoma, and fibrous dysplasia. Secondary bony lesions can metastasize from the prostate, thyroid, lung, breast, kidney.
Orbital tumors can also be linked to the lacrimal gland. These masses are fairly straightforward to diagnose using ultrasonography. Lacrimal gland tumors usually require steroids, biopsy, or excisional surgery. Lacrimal gland tumors may be bilateral or unilateral masses, adenoid cystic carcinoma, pleomorphic adenocarcinomas, and lymphoid masses. The types of lacrimal gland tumors are provided below:
- The majority of lacrimal gland masses are bilateral masses and are usually tender. Examples include sarcoid/pseudotumor or lymphomas.
- Unilateral lacrimal gland masses can be more threatening and may require a biopsy to determine malignancy.
- Adenoid cystic carcinoma is a malignant lacrimal gland tumor (epithelial) likely to require surgical intervention. They can recur years later and are associated with a very high mortality rate.
- Pleomorphic adenocarcinomas are aggressive lacrimal gland tumors. They are malignant growths seen in patients in their 50s and 60s. Treatment is surgical; however, there is a 75% mortality rate associated with metastases within 5 years.
- Lymphoid masses should be followed by a pathologist to determine the stages of disease. Treatment recommendation include chemotherapy, radiation, or both. Bilateral orbital involvement of lymphoid masses is associated with poor prognosis.