Orbital and Skin Tumors
Jump To
Idaho Eyelid and Facial Plastic Surgery manages diagnosis and treatment of both orbital and skin tumors in Boise, Idaho. An orbital tumor is any tumor that occurs within the orbit of the eye. It is typically not visible unless the tumor starts to erode the bone. A skin tumor is a cyst or lesion which is usually visible on the face. Both orbital and skin tumors may require biopsies to discover the nature of the growth.
What Is an Orbital Tumor?
The orbit is the structure that surrounds the eye and provides protection to the entire eyeball, with the exception of the exposed eye. It is lined by both bones and tissue contains the eyeball, its muscles, blood supply, nerve supply, and fat. Tumors can develop in any of the tissues surrounding the eyeball and can also involve the orbit from the sinuses, brain, or nasal cavity. Orbital tumors can affect adults and children. It can spread from other parts of the body. Mostly, orbital tumors are benign.
Idaho Eyelid and Facial Plastic Surgery’s surgeons are some of the few Idaho providers who are trained to manage orbital tumors, making our practice a top choice should patients suspect a growth within the orbit of the eye.
What Causes Orbital Tumors?
Orbital tumors develop differently in children and adults. The most common orbital tumors in adults are blood vessel tumors, including hemangioma, lymphangioma, and arteriovenous malformation. Tumors of the nerves, fat, and surrounding sinuses are less frequently occurring. Metastatic tumors most often travel from the breast and prostate. Squamous and basal cell cancers can invade the orbit from surrounding skin and sinus cavities. Lymphomas are the most frequently occurring malignant orbital tumors in adults.
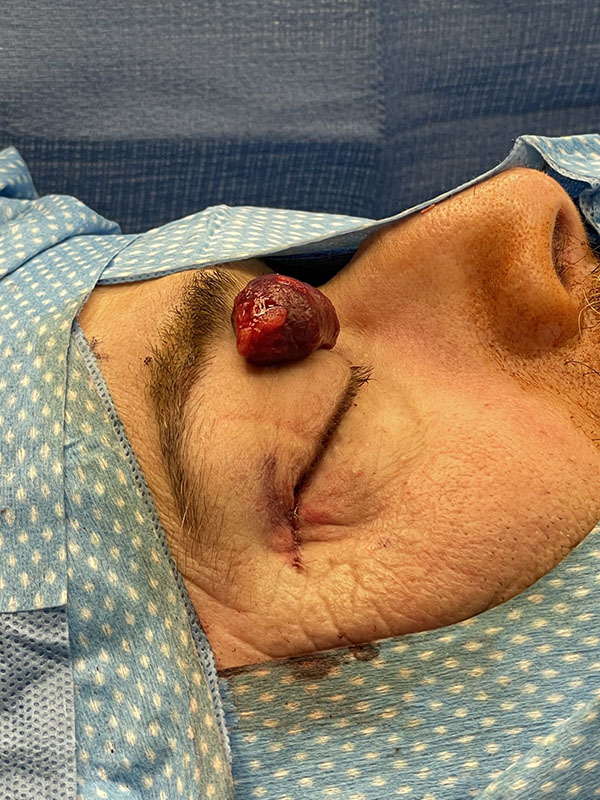
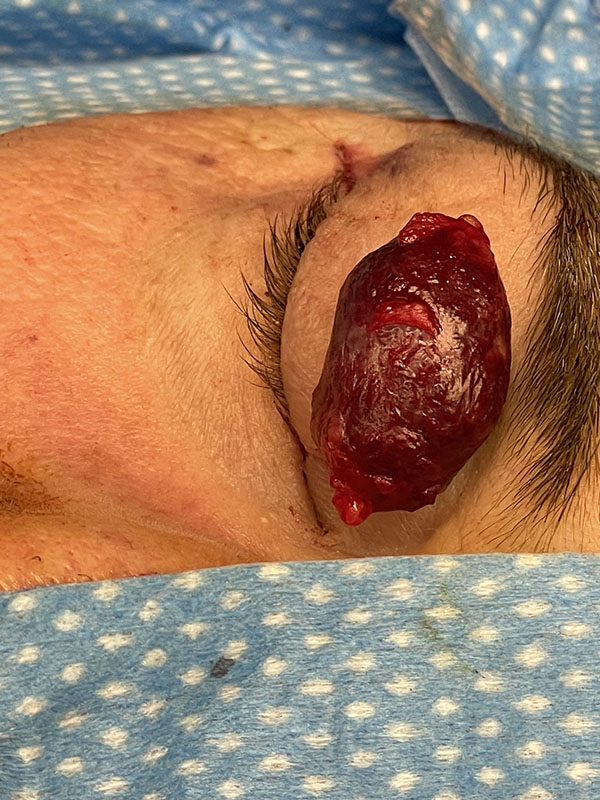
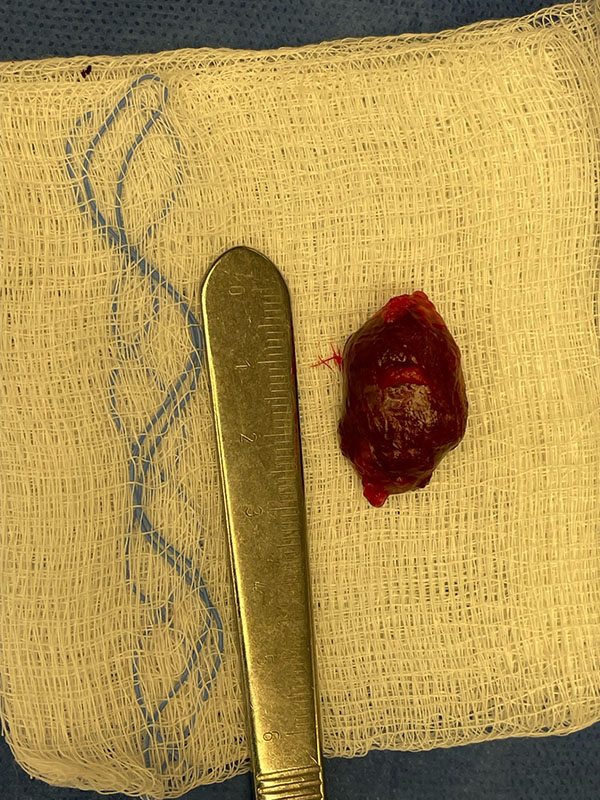
Benign Cavernous Hemangioma extracted from behind a patient’s eye
Orbital tumors present differently in youth. Most childhood orbital tumors are benign but can lead to developmental abnormalities. Common orbital tumors in children are dermoids, which are cysts of the lining of the bone, and hemangiomas, which are blood vessel tumors. While malignant tumors are unusual in children, any rapidly growing mass should be monitored by a specialist. Rhabdomyosarcoma is one of the most common malignant tumors impacting children. This type of sarcoma typically appears between the ages of 7 and 8.
What Are the Symptoms of an Orbital Tumor?
Symptoms of orbital tumors vary, but may include: protrusion of the eyeball (proptosis) from the pressure of the tumor, associated pain, loss of vision, double vision, swelling of the eyes, and redness. Sometimes a patient may observe an obvious mass just beneath the skin depending on the location of the tumor.
Note that eye protrusion is not always related to orbital tumors. Inflammation may point to other conditions such as Graves’ thyroid disease.
How Are Tumors Diagnosed?
After an initial medical exam at Idaho Eyelid and Facial Plastic Surgery, if our surgeons suspect an orbital tumor, they will order a patient either a CAT scan or an MRI. If results from those tests are suspicious, a biopsy can be taken to ascertain the nature of the growth.
How Are Orbital Tumors Treated?
The size, location, and type of the orbital tumor are factors considered when determining treatment options. While some orbital tumors require no treatment, it is best to continue monitoring them. Other orbital tumors are treated medically or with the use of radiation therapy. Some might require total removal by an orbital surgeon or a neurosurgeon, depending on the location of the growth. Additional radiation or chemotherapy might be required after removal. Note that in recent years, surgery is much safer because the CT scans/MRIs provide more precise tumor location and size. Our surgeons at Idaho Eyelid and Facial Plastic Surgery can help patients navigate this process to minimize risk and facilitate best results.
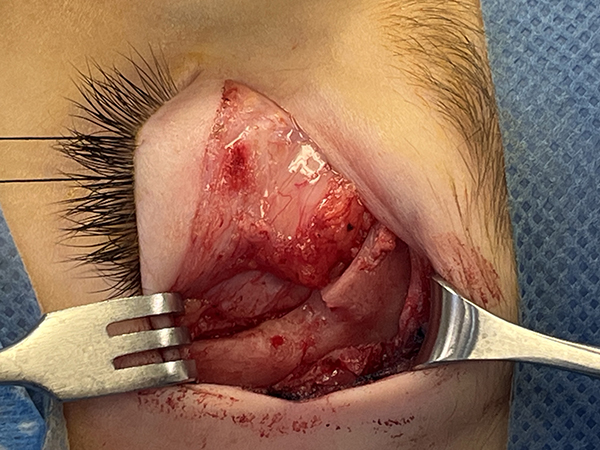
Pediatric orbital mass with bone destruction and bony rim reconstruction
What Is a Skin Tumor?
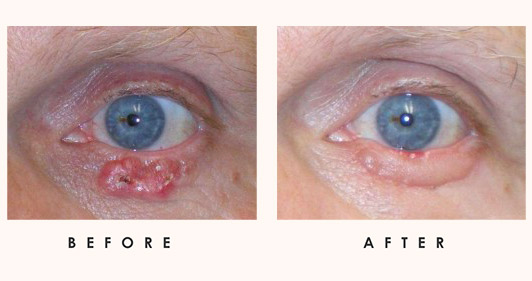
Cancer of the eyelid can be benign or malignant. Eyelid tumors can be benign cysts, inflammatory lesions, vascular lesions, benign epithelial lesions, pre-malignant lesions, viral lesions, and malignant lesions. Idaho Eyelid and Facial Plastic Surgery has extensive experience diagnosing and treating skin tumors and can help determine the nature of these cysts/lesions both through observation and biopsy.
To determine the precise nature of tumor growth, we look at a number of factors, including: eyelid growths/lesions that are pigmented or increased in size, eyelid moles/birthmarks with irregular border and changes in size, thickness, or texture, and/or a sore spot on the eyelid that refuses to heal.
Benign Eyelid Lesions
Benign Cysts
Benign cysts include epidermoid cysts, dermoid cysts, sweat ductal cysts and epidermal inclusion cysts. These are easily treatable, though the treatment option for each varies. Some of these lesions can be monitored, but many patients prefer to have them excised as they are an aesthetic nuisance.
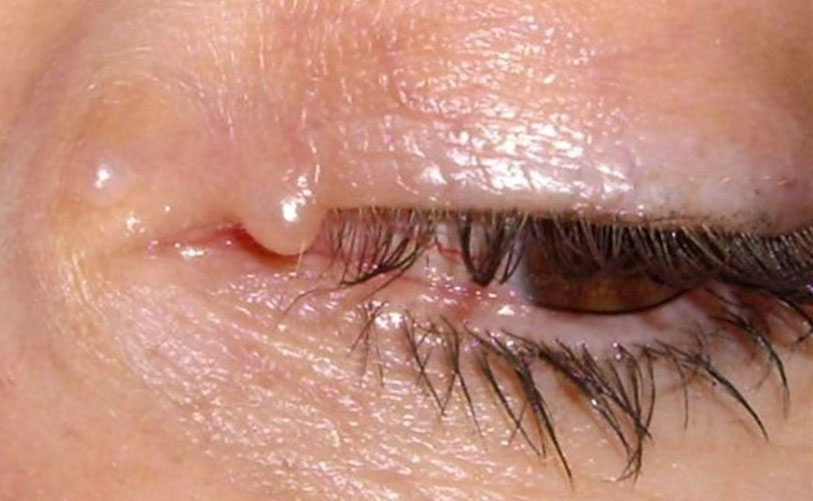
Benign Cyst
Inflammatory Lesions
Inflammatory lesions are not actually tumors, but they must be evaluated making a diagnosis of cancer. Inflammatory lesions include hordoleum (stye), chalazion, and parasitic infections. Styes usually require antibiotics and surgical drainage. Chalazion benefits from simple observation and hot compresses along with gentle massage. Parasitic infections may require anti-parasitic medication.
Vascular Lesions
Vascular lesions can look like eyelid tumors, and are called hemangiomas. They are either capillary hemangiomas, cavernous hemangiomas, or lymphangiomas. Vascular lesions are often seen in infants and children. If they are observed, they need urgent treatment as they can impact vision and can lead to blindness. Typical treatments include steroids, laser photocoagulation and surgical excision.
Benign Epithelial Lesions
Benign epithelial lesions are noncancerous growths. On the eyelids, they can be squamous papillomas, seborrhoeic keratosis, inverted follicular keratosis and keratoacanthoma. Squamous papillomas present as round with a smooth surface, and can be surgically removed. Interferons can also be used to treat papillomas: interferons are signaling proteins made by host cells in response to the presence of several viruses. A virus-infected cell will release interferons causing nearby cells to strengthen their defenses. Seborrhoeic keratosis is often monitored for a change in shape or size before any treatment is considered. Biopsies can confirm their benign nature.
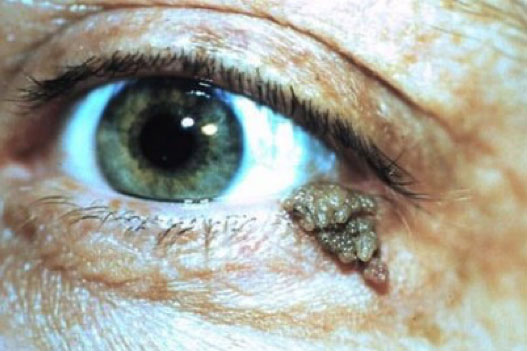
Squamous Papilloma
Pre-malignant Lesions
A number of different eyelid lesions can become cancerous, and include actinic keratosis, leukoplakia, xeroderma pigmentosum and radiation dermatosis. Actinic keratosis occurs in sun-exposed areas and appears like a white, scaly lesion. Excision biopsy aids diagnosis.
Viral Lesions
Common viral lesions include molluscum contagiosum, verruca vulgaris, herpes simplex and herpes zoster. Molluscum contagiosum is seen in individuals with low immunity, and can cause conjunctivitis. They are treated with cryotherapy or excision. Herpes simplex and zoster are treated with antiviral agents.
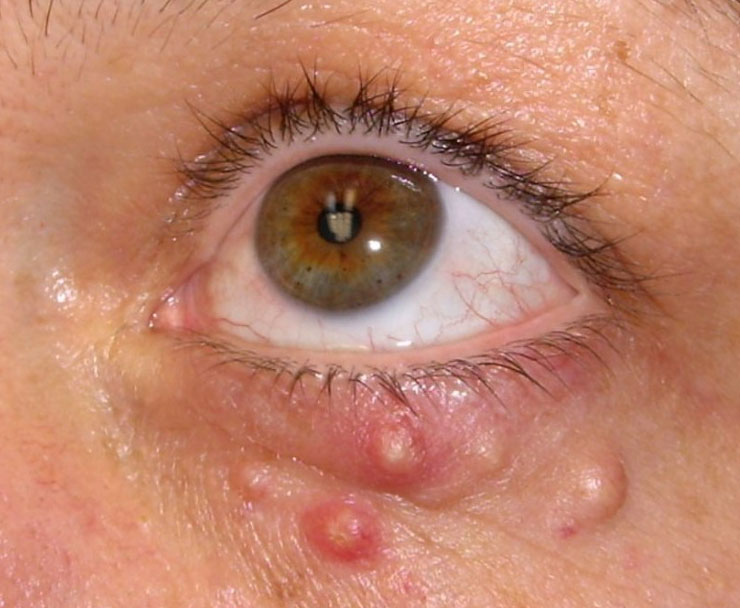
Ocular Molluscum Contagiosum
Malignant Eyelid Lesions
Malignant eyelid lesions are more serious and include basal cell carcinoma, squamous cell carcinoma, malignant melanoma and sebaceous gland carcinoma. Basal cell carcinoma is the most common eyelid malignancy, and sometimes occurs at medial canthus. They are locally invasive and require surgical excision. Squamous cell carcinoma is less common, and presents as red and scaly with an ulcer in the center. It should be excised quickly as it is vulnerable to distant spread. Sebaceous carcinoma is seen more in the elderly population, and can spread to lymph nodes and distant organs. Radical surgery is often needed. Melanomas are rare and often require excision.
Other Eyelid Lesions
Other eyelid lesions include xanthelasma, nevi and caruncular tumors. Most are benign and require simple treatments. Xanthalesma is associated with high cholesterol levels in the blood. Nevi tumors need excision if they change size or shape.