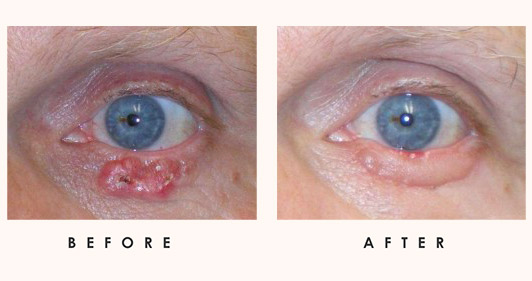
Benign Lesions
Jump To
Eyelid growths are classified into benign, inflammatory, vascular, benign epithelial, pre-malignant, common viral lesions and other tumors. These cysts and lesions are further detailed below.
Benign cysts
Benign cysts are abnormal growths filled with fluids or tissue, sometimes air. These growths do not pose a cancer risk. Benign cysts further categorized into epidermoid cysts, dermoid cysts, sweat ductal cysts and epidermal inclusion cysts. At Idaho Eyelid and Facial Plastic Surgery, these cysts are easily treatable, although treatment options vary.
Inflammatory lesions
Inflammatory lesions are usually inflamed or irritated. Although they are not textbook tumors, they pose additional risk when making a cancer diagnosis. These lesions include hordeola (styes), chalazia, and parasitic infections. Styes sometimes require antibiotics and surgical drainage, chalazion require observation and benefit from hot compresses and massage, and parasitic infections may need anti-parasitic medication.
Vascular lesions
Vascular lesions are abnormal growths of blood vessels. They can present as sores, ulcers, wounds, and even tumors. Hemangiomas are vascular lesions that can mimic eye tumors. They are subcategorized as capillary hemangiomas, cavernous hemangiomas, and lymphangiomas. When they present in infants/children, they require urgent care as they can lead to vision problems and blindness. Treatment usually includes steroids, laser photocoagulation, and/or surgical excision.
Benign epithelial lesions
Benign epithelial lesions can present as cysts, bumps, or papules. They include squamous papillomas, seborrhoeic keratosis, inverted follicular keratosis, and keratoacanthoma. Squamous papillomas are round and have a smooth surface. They can be surgically removed or treated through interferons, which are signaling proteins made by host cells in response to the presence of viruses. An infected cell releases interferons causing nearby cells to increase their anti-viral defenses. Seborrhoeic keratosis is observed for a change in shape or size before any treatment is considered. Biopsies can confirm that they are benign.
Pre-malignant lesions
Pre-malignant lesions can present some risk. Eyelid lesions that may become cancerous are actinic keratosis, leukoplakia, xeroderma pigmentosum and radiation dermatosis. Actinic keratosis presents in sun-exposed areas as a white, scaly lesion. Biopsies help in diagnosis.
Common viral lesions
Common viral lesions include molluscum contagiosum, verruca vulgaris, herpes simplex and herpes zoster. Molluscum contagiosum is seen in patients with low immunity and can cause conjunctivitis. While molluscum is treated with cryotherapy or excision, herpes simplex and zoster are treated with antiviral agents.
Other lesions
Other lesions are mostly are benign and require simple treatment. These include xanthelasma, nevi and caruncular tumors. Xanthalesma is associated with high cholesterol levels in the blood. Nevi require excision if they change size or shape.
When to Biopsy
At Idaho Eyelid and Facial Plastic Surgery, our surgeons have the expertise to know when to perform a biopsy for patients. We pay attention lesions/growths that: increase in size, have irregular borders, change in size, thickness, and texture. We evaluate pigment and all abnormalities that are sore and/or fail to heal.
Treatment
Removal through excision is a common treatment, especially when lesions/growths are on the eyelid and can obstruct vision and/or be a nuisance. Idaho Eyelid and Facial Plastic Surgery may have pathology check the tissue margins to be sure the tumor is completely removed. Alternatively, a dermatology surgeon may remove the tumor through Mohs surgery to ensure total removal. After Mohs surgery, reconstructive surgery is usually necessary. Reconstructive surgery is performed to make a new eyelid or repair the defect.
Reconstructive surgery is a strong area of expertise at Idaho Eyelid and Facial Plastic Surgery. The goal is to reconstruct the eyelid so that it functions properly, protects the eye, preserves vision, and has a satisfactory cosmetic appearance. Our patients should be aware that removal and/or reconstruction of eyelid skin cancer will leave a scar. An effort is always made to minimize scarring and obtain optimal cosmetic results. After surgery, the healing process may take six months to one year. Once the wound has healed, follow-up with your surgeon is necessary to be sure that the skin cancer does not recur. Should there be development of a new cancer, it can then be detected early and treated promptly.